Movement variability & its relation to pain and rehab.
Movement variability has definitely been receiving a bit more attention over the past year or so and coming into more and more discussions about movement. Anyone who has kept an eye on this blog will see it has been mentioned regularly over the past few years. If we explore the research into this area we see it has been a focus in academic circles for a great deal longer although it is filtering down at a glacial rate to training and rehab programs.
Hopefully we are starting to shift our understanding of the human body away from the mechanical and towards more of a biological perspective. This may help us to understand why changes in someone’s posture and ‘imbalances’ in general within the body don’t actually matter quite as much as they would in a purely mechanical system. The tolerances of the human biological system are probably much greater than we give them credit for.

Rage against the machine
Within the paradigm of a mechanical system, seemingly the predominant model taught today, the operation of the body is viewed as a precision machine. If one part of a machine breaks or operates outside of the precise narrow parameters set for it then it spells disaster for the machine as a whole. We often blame deviation from poorly defined ideals and ideal relationships within the body for various injuries and diseases when often they do not have clear correlations.
Pain and its relation to posture would be a perfect example of this, as would concepts such as ‘overpronation’ and muscle firing patterns and timings. Movement is just the same, there are not many ‘right’ ways to move that have been objectively defined and can therefore be blamed, instead we have wide parameters of what we can consider ‘normal’.
Humans are simply not like machines, they have a wide variety of ways in which they operate as well as different tolerances, adaptation and rates of adaptation. Metal will have a finite point at which it breaks whereas the body as a biological organism can adapt and increase its tolerances. Wolff’s law is a perfect example of this, as is going to the gym! Sometimes we can exceed these tolerances though as well as asking too much of our adaptive mechanisms.
Variations within movement have been traditionally viewed as ‘error’. These ‘errors’ are seen as redundant, no longer needed, and in the traditional model of motor control through practice this error is hopefully eliminated. A quite different view is now being put forward with the concept of motor ‘abundance’, the redundant elements now being seen instead as positive aspects of physical capacity to be utilised and indeed vital for movement. This paper “The bliss (not the problem) of motor abundance (not redundancy)” from Latash *Click Here* outlines this new view superbly.
When we are taught exercises we are shown the ‘right’ technique that has been designed to target a muscle based on the fixed ‘correct’ way a muscle contracts based on its static anatomy. The exercise is designed to be repeated, rigid and invariant for a specific outcome. A specific unvarying overload is the aim with the outcome of making something bigger and/or stronger. If movement is variable then so must muscle function be to! This basic reality is left out when we are taught about anatomy and movement, perhaps it is too complex for the mechanical model!
Bernstein’s original studies in the 1930’s into Blacksmiths striking a chisel with a hammer found experienced task-based workers to display “repetition without repetition”, the striking and hammer trajectory displayed low variability vital to a stable repeatable performance. The end point of the skill was the same but the joint angles and segmental variability was high.

This segmental variability is called the coordinative variability *Click Here* This is vital to an ability to maintain performance and not break down due to the specific overload a repeated performance of a skill may incur. This would be very relevant to running for example and decreased variability and patellofemoral pain is discussed *Click Here*
The runners in the PFP group displayed tighter coupling (less variability) between segments whereas a looser coupling was the norm in the healthy group.
Seay et al *Click Here* found differences in variability between groups who had suffered on going LBP, single bouts of LBP and those who had never suffered LBP. The differences in variability between those injured, recovered from an injury versus those never injured may gives us valuable insights into elements that may need to be focused on in rehabilitation.
We will discuss this in greater detail later.
Their conclusion was:
“Taken together, the data lend insight into increased injury risk and performance deficits associated with even one bout of low back pain, and suggest that clinicians need to look beyond the resolution of pain when prescribing rehabilitation for low back pain”
Movement variability is inherent within a biological system. Not only is it inherent it is also beneficial for reducing risk of overload and enabling the ability to adapt to events that occur within our ever-changing environment. Elite athletes cannot reproduce exact and invariant movement patterns repetitively even through hours of devoted practice. The best movers are those that can execute the same stable end point skill but in many variable ways dependant on the constraints and context of performance. It could be that part of being resilient and robust lies in variability. The ability to tolerate load may come in part in the way in which it is internally processed through our coordinative variability.
Movement is often studied and the data homogenised to reflect a measure of the group being studied. We should also look at the inter (between) people and intra (task to task variation) information as well to better understand the wide ranges of movement variability that exists and what this may tell us rather than this vital data being swallowed up *Click Here*
Here is an example of 5 single leg squats collected by me from the same person using wearable motion sensor tech. Each one is subtly different for the measures taken.
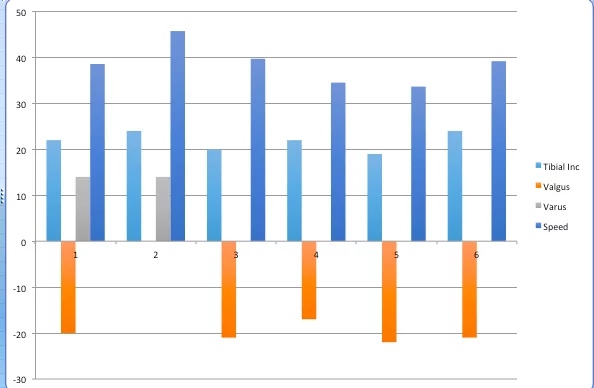
As a little self driven experiment try signing your name repetitively 10 times in the same place. How many of them are exactly the same? They will be similar around the same general outline but never exact and this will be a movement you have practised thousands of times.
Vital for rehab
So why does all this matter to rehab?
Simply put pain changes movement.
Lets start by looking at pains affect on movement variability where we find a significant relationship. Any rehabilitation program should look at the effect of pain on the subsequent function of the individual. Targeting deficits in functionality that are highlighted by research should be regarded as ‘best practice’ during rehabilitation.
Adaptations to movement during a pain state can often be beneficial; a limp is a great example of that decreasing the load to the injured tissue through changing movement patterns. These changes may not be only in a specific pattern of avoidance but also the speed, range and variability of movement. The system can create ‘protection’ through increasing mechanical stiffness and decreasing the variability of movement the injured area and associated areas go through.
Here is a new paper from Hodges outlining some of these changes in more detail *Click Here*
Here is one of my favourite quotes
"Adaptation to pain has many short term benefits but with potential long term consequences" P Hodges - Moving differently in pain 2011
The problems come when the short-term benefit is no longer beneficial. This can be described as maladaptive. The goal of protection is no longer necessary but no one has come along and told the system that quite yet!
Long term consequence of movement maladaptation at a tissue level can be increased load to certain tissues and deconditioning in tissues being used less thus increasing risk of overload, especially if this strategy now becomes invariant.
On a cognitive level we may start to see factors such as fear avoidance behaviors reduce the variability of someone’s movement. A top down (cognitive) based approach may also be useful for helping people to become more variable again. A combined top down and bottom up (physical movement) is a promising way to address two elements that are implicated in a successful rehabilitation.
Zusman here outlines an excellent process *Click Here*. Creating new, different, and novel memories to be used would be an aim of rehab using this combined process. Nijs et al also outline a similar process here *Click Here*
An invariant strategy may also lead to repetitive proprioceptive information that has become coupled with pain and specific movements at a neural (neurotag) level reinforcing the pain experienced and maintenance of that pain. I discuss the concept of ‘pain memories’ here. *Click Here*
Moseley and Hodges discovered that movement variability was linked to cognitive factors. They found that for those that experienced a decrease in postural variability after experimental pain that normal resolution of their original postural strategy did not occur and was also linked to their cognitive beliefs about back pain.
This may affect both continuation and reoccurrence of back pain and was discussed in the article as a potential risk factor for the development of chronic LBP. *Click Here* We also see this from Jacobs et al *Click Here*
Decreases in movement variability are associated with chronic pain consistently in the literature and I will explore some more of it below. Acute pain is associated with an increase in movement variability. This is theorized to be due to the motor system trying to find non-painful movement variations. If someone does not have a system capable of varying its movement then finding alternative strategies may be problematic and thus possibly lead to chronicity.
As a potential predisposing factor for chronicity of an injury we must both see it as a key rehabilitation component for chronic injury and also a prophylactic measure to help prevent the transition to chronicity. Certainly it may give us some insight into why previous injury has an effect on future analogous injury.
Debra Falla’s group *Click Here* took nineteen CLBP sufferers and matched them against age and gender controls during a repetitive box lifting task. The CLBP group displayed altered movement including reduced movement from the spine hypothesized to be due to increased stiffening of the spinal region. Another measure they took was EMG activity of different portions of the lumbar erector spinae. They found that the CLBP group performed the task using the same portion of the muscle. In contrast the control group activated different regions of the muscle at different times during the task. The non-varying strategy of the CLBP group was associated with increased pressure pain sensitivity of the lumbar area. They theorized that
“Reduced variability of muscle activity may have important implications for the provocation and recurrence of LBP”
This paper *Click Here* looked at the running kinematics of twelve individuals with a chronic Achilles tendon injury vs twelve matched uninjured control subjects. They found the entire Achilles injury group displayed a “distinctive and consistent pattern of loading” whereas the control displayed a markedly different pattern of variation with increased levels, in essence a higher degree of variability.
This study *Click Here* looked at female runners who had had a previous tibial stress fracture and they were compared with mileage matched uninjured female runners. They then looked at their inter limb variability (coordinative variability). The previously injured runners displayed decreased hip-knee and knee-ankle (the largest effect) variability in the injured limb compared to the uninjured limb. The controls displayed no difference between limbs.
Decreased variability could be potentially be both a cause and effect of pain. Stergiou in his paper "Human movement variability, nonlinear dynamics, and pathology: Is there a connection?" explores this question.
Decreased variability as a causative factor in the absence of a previous event certainly needs exploration through future prospective studies. This paper *Click Here* looks at movement variability in stereotypical occupational activities and the risk that reduced variation may pose.
To be variable we probably need well functioning and reasonably accurate basic movement hardware such as the proprioceptive system and cortical areas associated with movement. It is well documented that these are both affected by pain. We then need to couple this with a memory bank of movement experiences and skills that form what I term a basic ‘movement vocabulary’ that allow us to be variable and adaptable to different situations and variable stimulus. These basic movement skills are also often missing after injury especially in those with a chronic injury or pain.
As I have gone on for quite a while here I will expand on a few of the aspects discussed here in a second part to this. I would like to go into more detail on the neural aspects involved in variable movement as well as expanding on end point and coordinative variability. I will also address some basic ways of increasing variability in a simple, easily applicable and practical way.










Leave a Reply
Want to join the discussion?Feel free to contribute!