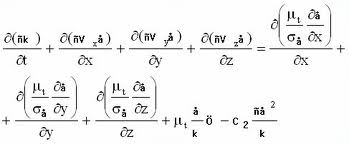Now this post equally could have been hip pain, knee pain or foot pain when running. The available motion in the big toe or hallux will affect the operation of all of these body structures during integrated movement.
Read more
Things have been really busy with Cor-kinetic recently and I have not had a lot of time to blog. This post stems from a case I have been dealing with recently and I wanted to give an idea of our thought process at Cor-kinetic and how the symptom and cause of a problem are not always one and the same.
The patient in this case has been having Achilles problems on the left side and also lateral foot pain on the same foot. Interestingly the pain reduced the quicker he ran but more about that later.
Read more
At Cor-Kinetic one of our foundational concepts is that of the relationship between stability and mobility.
Stability is a component part of mobility. The body needs to move in a mobile AND stable manner. Stability without mobility is RIGIDITY. Rather than a sign of functionality of the system I would see it more as a sign of dysfunction. The inability of our motor system to effectively control movement will create a rigidity in the system as the body chooses stability over mobility and closes down the system's ability to move.
Read more
Whenever we run a Cor-Kinetic course for physio's and other health care professionals the same subject always comes up, the TvA and lower back pain (LBP). This inspired me to write a blog on the subject!
Read more
I had an interesting case this week involving a water polo player who was experiencing shoulder pain when throwing. This pain was only occurring however when he put maximal effort into the throw. Now I do not get to see many water polo players so this was a challenge. I decided to put aside the fact that ground reaction forces would be different as well as having two different resistances on the upper and lower parts of the body (air and water friction) as this would present even more challenges to the assessment!
Read more
So its been a while since I last wrote a blog. Been pretty busy moving house and working hard so had very little time.
This blog is all about the movements that we give our patients/clients to perform and how we may need to pay closer attention to how they do it for maximum impact on the system.
One of the things we look at heavily during the Cor-Kinetic Mentorship program is the reaction created by the movement we perform. Just because we believe that a movement we prescribe will enhance our clients movement does not mean that this movement will give us the reaction we desire.
Understanding the authentic biomechanical movement that we need in the first place is only one half of the battle. If it was as simple as that then very few people would be in pain. How much of that movement does some one tolerate is the question, and to find the answer we need to look at their movement threshold.
If we have too large a movement into an area that lacks the required movement then you will get a compensatory movement from the body. It is as simple as that. The response you thought you would get will not occur. In fact it could be this compensation that is causing the pain you are trying to eliminate. This is why it can be hard prescribing corrective exercises. You don't know if you are feeding the compensation beast or correcting a movement! The more we go towards end range the more the variability of the response becomes. As the demand/stress increases so does the bodies need to find an alternative pathway.
Along with patient adherence this has always been the problem with corrective exercise prescription for the client to go away and perform on their own. This is where the science of the body meets the art of the practitioner. As the body is not a linear system and does not follow a set pathway every time it moves we have to be able to interpret and control movement at the moment it occurs and be able to adapt movement for a favorable reaction. Not always and easy thing to do but hugely powerful once you can start to implement this thought process.
To guarantee that the reaction we need to find the threshold of success. This is a concept borrowed from the great Dr David Tiberio of the Gray institute. The threshold is the point that the movement can still have a positive reaction the vast majority of the time and will remain pain-free. The more we go over the threshold and suddenly the movement becomes unsuccessful as the body tries to find another pathway or creates pain to reduce the sub optimal movement created. The key is feed the body a little more demand each time. Inching over the threshold bit by bit until we have a consistent positive reaction. Understanding the range, angle and speed of the movement can help you increase and decrease the variables to be able to have full control over the patients/clients success and being able to increase it. It maybe that the threshold we have in terms of range will decrease the faster we get. This maybe of great importance for a sports player who has to increase their movement speed.
An example of this process would be a lunge for increased pronation of the foot. If we were stepping with the right foot then we would want to step across to the left half of an imaginary semi-circle in front of me (somewhere around 45 degrees left would be good!). If the body cannot get this movement under increased force then it will try to decrease the impact on the system. A couple of ways it may do this is simply to roll to the outside of the foot or adduct the foot (turn it in). In these ways it reduces the demand on the structures that would get eccentrically stressed during pronation (Tri plane-dorsi flex, abduction, eversion) . We need to be able to find the threshold or angle that decreases these compensatory reactions and progress slowly until we have the angle and reaction we need/desire. A better angle to start at maybe 10 degrees gaining a consistent reaction before moving to 20 and so on and so on. When the reaction becomes less consistent we can come back to success and start inching over the threshold degree by degree. It may sound time-consuming but is actually a quick process when you learn to control it!
In this way we can regress and progress the movement to create continued success. The more the body feels and interprets this success the more we can feed the neurological system to allow the continued success to become a predominant pathway of movement. It is not always the movement we give but the way in which we give the movement!
As the great Gary Gray says "The test is an exercise and exercise is a test". In this way we can interpret the success of any movement we perform and constantly evaluate the success of the individual we are training/assessing/treating.
A purely academic/biomechanical approach to functional movement may lead us just to understand what movement is required and give as much as possible. This is something I have seen many times with a fairly low-level of success. The variability in the creation of the desired movement is high. At Cor-Kinetic we don't see that as the answer. In fact in this scenario more can actually lead to less, the path to success is in the way that you do it. Our tag line is "Evolving movement" both our students understanding of movement and our clients movement potential.
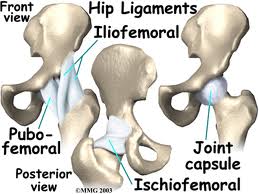
At Cor-Kinetic we appreciate the power of the hip capsule and specifically the capsule ligaments. How to stimulate the capsule forms a component part of what we teach both academically and also in terms of technique.
We find that the powerful effect that capsule stimulation has on the muscles surrounding the hip-joint means that it is an area of the body under recognized when looking to create motion and stability around the hip and subsequently the body as a whole.
Anatomy
The three extrinsic capsule ligaments are arranged in a helical structure. This means that each ligament may respond to motion in any of the three planes of movement. The illiofemoral ligament is the largest and strongest. In fact it is the strongest ligament in the human body!
Why?
Ligaments are highly proprioceptive. This means when placed under tensile forces they send lots of information back to the CNS (central nervous system) and also surrounding musculature. If we get into a scenario where the hip muscles restrict motion around the joint then the capsule stops becoming stimulated. This is a bit of a catch 22 because if the capsule stops getting stimulated then it will not in turn play its role in stimulating the muscles surrounding the hip. This leads to a 'locking down' of motion in this area. As an area of huge mobility and freedom in the body (as a ball and socket joint allows) it can then impact on areas such as the lumbar spine, sacroiliac joints and general lower back area that rely on the motion and force dissipation of the hip and associated muscles for correct sequencing of movement and healthy operation.
Research
Solomonow (2003) has documented much of the research into the proprioceptive ability of ligaments. Multiple anatomical studies have shown the presence of Pancinian, Golgi and Ruffini mechanoreceptors within ligaments. This means that through stimulation or lack of stimulation the capsule ligaments can create reflex activation or inhibition of the associated musculature. As far back as 1900 (Payre) it has been suggested that a reflex arc exists between muscles that may directly or indirectly modify the load imposed on a ligament. In this way the body can create a synergistic activity of ligaments and muscles for joint stability/mobility. The indirect nature of this reflex arc also shows the functional inter-connectedness of the body that we often miss with a joint-by-joint isolation approach.
This reflex arc has not just been noted in the hip. The stimulation of the medial collateral ligament of the ankle results in activation of the intrinsic muscles of the foot (Solomonow 2002). This again shows the power of the functional chain as many of these muscles do not cross the ankle joint! As we already know, during the pronation cycle rotation around the STJ (subtalar joint) is accompanied by rotation at the MTJ (midtarsal joint). This motion at the MTJ will also help decelerate lower limb motion preventing excessive motions at the knee and hip.
Traditional lengthening of muscles may not be the answer to create more motion at the joint to create more stimulation of the capsule. As muscles get towards end range they become stiffer (more resistant to lengthening), similar to what would happen when we stretch an elastic band. This would mean that the stress (force divided by area) applied would not result in strain deformation of the tissue or more simply put lengthening. This may mean that the capsule ligaments, which would be stimulated more towards the anatomical end range, may get reduced input. Both muscles held towards end range and muscles held shortened could display increased stiffness. Gadjosik (2002, 2003, 2005) has performed research into stretching and increased muscular stiffness.
Method
Our methodology, especially around the hip, to create more capsule stimulation involves creating a passive shortening of the muscle in the transverse plane. At Cor-Kinetic we believe the transverse plane is responsible for a lot of the intrinsic stability in the body. Much like the ropes of a ship's mast, when we rotate or 'wind' a longitudinal oriented structure/muscle (also longitudinal orientation of the individual fibres), we create a passive tension. This tension is created quickly in a plane (such as the transverse in a longitudinal muscle) that lacks much range. This range would be much larger and therefore more movement before a stiff response if deformed longitudinally rather than rotationally. This would mean the stiffness/tension and resultant stability on offer would take longer to access.
To avoid this lengthening and resultant stiffness we instead 'unwind' the transverse plane by externally rotating. As we know from our anatomy lessons there are many more external rotators around the hip than internal rotators. We tend to rely on gravity for internal rotation during functional movement!
We can further reduce stiffness by creating stability. Instability tends to create rigidity (increasing stiffness) around a joint therefore reducing movement and capsule stimulation. Simply pre-positioning our bodies towards the anatomical end range will also help create capsule ligament stimulation.
So our three golden rules of capsule stimulation at Cor-Kinetic are to shorten the transverse plane to reduce stiffness, create stability to reduce stiffness and preposition further towards end range. By changing body position and drivers of movement we can emphasis motion in the individual ischiofemoral, iliofemoral and pubofemoral ligaments. This should result in more stimulation of the highly proprioceptive capsule ligaments for reflexive stimulation of the associated musculature.
Simply not enough!
Stimulation of the capsule however is only one part of the story. Following this muscular activation 3D mobility must then be restored to the joint. This mobility must then be integrated into our movement. To much mobility maybe shut down by the body as it could be beyond the perceived range of the proprioceptive system. By introducing dynamic and integrated movement we can teach the body to understand this motion and create stability and strength in its new-found range and therefore integrate this motion into its everyday movement patterning.
This maybe why manual therapy techniques can be short-lived as we do not teach the body to stabilize the new-found joint mobility and mobility is perceived as instability. This is why mobility must be integrated into actual movement to create stability. Gary Gray has coined the phrase "mostability" to describe this process.
We teach a 3 stage 3 dimensional mobility/stability process on our two-day courses along with assessment techniques to determine which areas need to be focused on!
For more information on our courses please click this link Cor-Kinetic education.
As always this is our take on complex subjects and merely opinion back up with a smattering of research.
One of the key things to understanding how to view the body functionally specific is the biomechanics behind how we move.
A (simplified) understanding of biomechanics allows us to break down different functions to create authentic movement based techniques that create the right joint reactions for when we are training or treating our clients. After teaching a mentorship group last weekend some of Cor-Kinetic’s principles of biomechanics I thought I would write this blog post to help explain our process that has also been influenced by the teachings of the Gray institute.
Now the word biomechanics sounds a bit scary. If you have ever opened up a biomechanics book or journal then you will probably have had a similar reaction to me, which is one of amazement at the equations and symbols on offer!
(Apparently the biomechanics behind swimming!)
Instead in the process we use at Cor-Kinetic we are looking more at the movement of bones both in real space and in relation to each other. This relative movement of the bones creates specific joint reactions that in turn will have an affect on the attached muscles for an authentic reaction in the neuromuscularskeletal system as a whole.
The real key is in understanding that the real bone motion and relative joint motion can be different. So in essence we could have two bones both externally rotating in real space but the relative motion between the bones at the joint could be internal rotation. This hinges on the difference in speed between the two bones. Lets outline some of the key points below.
Proximal and Distal.
It is key to know which is the proximal and which is the distal bone at a joint.
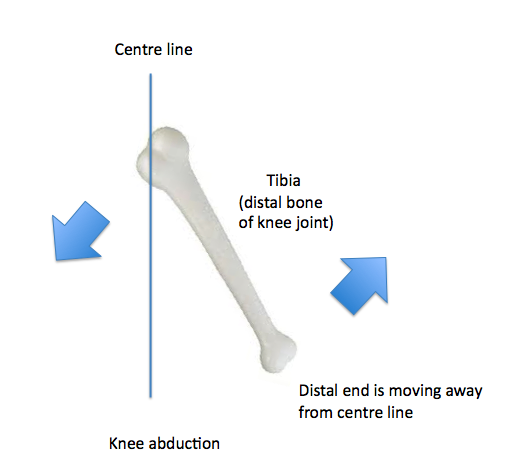
In the appendicular skeleton (extremities) the motion the DISTAL end of the DISTAL bone is going through RELATIVE to the PROXIMAL end determines joint motion. This means if the proximal end is moving towards the centre line in the frontal plane for example then the distal end will be moving away or abducting!
The distal point of the Axial skeleton is also known as the superior point. So now we look at the superior point to define joint motions at the axial skeleton.
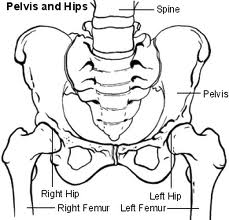
The proximal bone is the one that is closest to the centre of the body. Therefore the pelvis would be the most proximal bone of the body. The other bones are distal to it. That makes understanding the proximal and distal bones of the hip joint easy as the pelvis is always proximal. At the knee the femur would be the proximal bone to the distal tibia.
The motion of the pelvis is also determined from a different point. Rather than the distal end (because both are!) we look at the relative movement between the ASIS and PSIS. Anterior rotation would be the counter-clockwise rotation of the ASIS so the PSIS would be superior to the ASIS.
The same counter-clockwise rotation as we see from the tibia would be described as posterior rotation because the distal end has rotated towards the posterior. This can sometimes be confusing because both the tibia and pelvis bones are going through the same rotation but one is described as anterior and the other posterior!
Relative speed.
The relative speed of the two joints is also critical to determining the relative joint motion.
It is important to now know which bone is moving faster as this will help to determine the relative joint motion. The general rule is that the closer the bone to the driver of motion the faster it will be going. This is because of the dissipation of force. As an example, a foot driven motion will generally mean the distal bone of the lower limb will be moving faster. So at the knee the tibia will be driving faster than the femur. If we were to hit a tennis shot however the proximal femur would be closer to the driver of the hand meaning it will be moving faster. At the elbow however the distal radius would be closer to the hand meaning it would be driving faster than the more proximal humorous. So we need to know the driver and which of the bones that comprise the joint we are looking at is closer to the driver.
There are 3 real ways a joint can move in function (and two more less functional to make 5). This would be proximal and distal moving in the same direction, proximal moving faster. Proximal and distal moving in the same direction, distal moving faster and then proximal and distal moving in opposite directions. This would be either towards or away from each other as if we view a clock face movement towards each other would mean one was moving clockwise and the other counter clockwise this would be the same when moving away from each other also!
This is all very easy when the distal bone is moving faster as the real bone motion and relative joint motion will be the same. The confusion comes in when the proximal bone is driving faster than the distal in the same direction. In this case the relative joint motion will be the opposite to that of the proximal bone. An example in the transverse plane would be at the hip in the back leg of gait. Both the real bone motion of pelvis and femur is rotating in the same direction, externally. However because the proximal is rotating faster the relative joint motion is internal rotation. The easiest way I find is to put my fists on top of each other. I then rotate the proximal bone in the direction it is rotating, in this case external. I then rotate the bottom hand in the opposite (what determines the joint motion) and this is internal! The transverse plane can be easier to understand sometimes because the whole bone will be rotating in the same direction rather than the proximal end one way and the distal end the other!
One movement that can sometimes be confusing is abduction of the knee. This is because the largest motion is from the proximal end going towards the mid-line, rotating around the axis that runs posterior to anterior. But if we follow the rule of naming the joint motion from what the distal end of the distal bone is doing relative to the proximal end, then it is moving away from the centre line of the body or abducting! Easy when you know the rules!!
Check out www.cor-kinetic.com for more information on our courses.
As always this is an example of our thought process rather than a defined way that things have to be done in an academic sense! We hope it helps!
I have been reading The Talent Code this week by Daniel Coyle and have enjoyed it immensely. One passage in the book stood out to me. It describes the difference between how we teach football and how we teach musical instruments, specifically the violin.
"The ideal soccer circuit is varied and fast, changing fluidly in response to each obstacle, capable of providing a myriad of possible options that can fire in liquid succession: now this, this, this and that. Speed and flexibility are everything; the faster the more flexible the circuit, the more obstacles can be overcome, and the greater that players skill"
Now that sounds pretty cool. So if we want to help improve someones soccer (football) circuit then our training for that sport should help increase the sphere of the players movement, speed and flexibility. To be dynamic, variable and increase the brain/body connection would seem prerequisite for such an activity. This would be a functional approach to training!
BUT in fact Coyle goes on to talk about how we teach people to play instruments, in this case the violin.
"This circuit is not a vinelike tangle of improvisation but rather a tightly defined series of pathways designed to create-or more accurately, recreate-a single set of movements"
This struck me as a more accurate description of how we teach people to exercise in the gym. A set way of performing a movement not to be deviated from. A series of movements that lack the variability of any sporting or movement skill that we may want to enhance, in fact a completely different skill set.
When we build neural circuits and fire them repeatedly they get larger, stronger and after time and repeated use through practice they get myelinated. The Myelin insulates the circuit allowing the signals to travel faster and more efficiently. These circuits are specific to the practice or training the we do. Playing the violin does not increase my skill or ability to move or produce force for football.
The generic nature of exercise and strength training in particular would lead us to believe that strength and movement are generic. By practicing a defined pathway movement such as a squat this will enable me to improve the incalculable movement and strength/force production variations involved with football. The deadlift and bench press, movements that do not move my centre of mass away from the vertical, will enable me to explode in various directions and apply my force against another body in the horizontal plane. Studies have shown very limited crossover from training one specific movement to another specific movement!
The variables involved in applying your force against a moving external object are huge. From the foot positions taken to the change in position of the opposite body and the angle both bodies are moving in.
During a specific functional activity the feedback loop from the nervous system will define the appropriate response in terms of movement and ability to apply force. If the circuit is not variable then can it respond to a varied input?
Mel Siff states:
"The rate and number of fibres firing depends on voluntary and involuntary processes....the involuntary ones to the feedback of the proprioceptive system"
Involuntary would be more subconscious processes that are involved in sporting activities. They would also apply to the stretch reflexes involved with eccentric before concentric contraction! Something else involved with sporting force production.
Siff also states:
"there will usually be changes in centre of gravity, moments of inertia, centre of rotation, centre of percussion and mechanical stiffness of the system that will alter neuromuscular skills required in the sport"
If we believe that the mechanical/neurological skill process is vital to specific functional force production or strength and that during sport this is a constantly changing and evolving landscape then to train for this process we must involve variability. It must be more like teaching someone to play football than the violin. More variable than defined.
We must allow the body and mind to process information and create a response based on that information. Instead we try to create a robotic series of defined motions that offer a limited response. Even worse at an elite level of training we have created governing bodies that advocate training protocols with exceptionally limited variation in exercise. None of which ever come away from the vertical, none of which involve rotation. Sound like sport?, look like sport? Seems to me it is more like playing the violin than football!
How many sports only involve moving the centre of mass in the vertical? The ability to decelerate and accelerate in the horizontal plane is pretty much sport! Throwing, kicking and hitting all involve rotation. They also all involve strength, flexibility, speed, stability and power during the same split second periods of play! Not as individual components.
A similar rationale maybe applied to the world of rehabilitation from injury also. Do we want to prepare our clients for a limited range of specific movements or the variability of the world that we function in. This would be a personal choice.
On a final note, Malcolm Gladwell in his book 'Blink' describes a complex war game in which he felt the protagonists over analyzed the scenario in front of them.
"They were so focused on the mechanics and the process that they never looked at the problem holistically. In the act of tearing something apart you lose its meaning"
I believe that this can happen in our approach to the body. By reducing it to components we lose the magic of integration that creates movement. This also leads us to understand why injury site and source may be different! If we focus solely on the injured component then the cause will never become apparent. This is in part why we have chronic problems.
As usual this is my own take on a complex subject. More opinion than fact! Although with supporting evidence.
Check out www.cor-kinetic.com and www.facebook.com/corkinetic
Ben
A term I tend to hear quite a lot in the gym is 'muscle firing'. A classic example of this is "I have been told my glute's don't fire." I must admit I am a little confused by this term.
As far as I can tell this term means muscle activation and this is where I start to get even more confused. This activation usually refers to a muscle shortening (concentric) and producing force. What we have to ask ourselves is, is this how muscles work?
In these situations I always like to refer back to my principles of muscle function. In this case specifically the principle of muscles lengthening before they shorten. This eccentric lengthening is the activation or trigger for the concentric force production.
This is a pretty solid principle. Go to throw a ball and first you rotate the opposite direction. Go to jump and first we go down. Even standing from a seat we flex forward before we extend. So if my muscles aren't firing is that because we have not given them the input (eccentric) to activate? Especially during function related and non-contrived movement away from the gym!
I have seen various muscle firing tests, many lying down while being palpated, usually with the diagnosis that the muscles are not firing properly or in sequence. Well what do you expect?? If we ask a muscle to shorten without first eccentrically lengthening as we see in functional movement how can we expect it to 'fire' properly?
Also what would the 'firing' sequence be when lying down. Different movement patterns will have different muscle activation patterns based on joint angle. As the angles change so will muscle activation. If my glutes are not firing when I lie on my front then that makes sense to me. No eccentric activation has occurred, nor is it likely to as my ability to flex is blocked by the floor (according to classical anatomy). We also have to ask ourselves what movements activate (lengthen) the glutes. If we look at the oblique angle of the muscle it would lead me to believe that internal rotation and adduction would also play a huge role. If we look down the body at the sub talar joint (STJ) the similar direction/angle of the joint (42°) to the glutes action line means that the joint moves predominantly in the frontal and transverse planes (Eversion and abduction). Why then do we see the largest glute, the glute max, as a predominantly sagittal plane muscle? In fact the relationship between the two parts to me is obvious. The axis of the STJ reacts to ground reaction forces going up and in, inferior lateral to superior medial, the glute action line will run perpendicular to this running down and out (pointed out by my good friend Ola!). A perfect relationship to help eccentrically decelerate STJ motion before producing force. In fact as the great Gary Gray calls the STJ "The switch that turns on the engine (glute max)." So for glute activation do we need to be upright and moving? I would say yes!
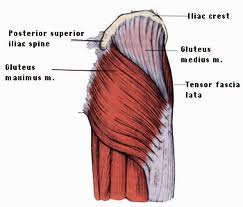
Here we can see the perpendicular relationship of the action line/striation of the glute from origin to insertion and the axis of the STJ.
How can someone tell the split second difference in activation between different muscles, especially through palpation, without the aid of expensive EMG equipment? What sequence are muscles meant to fire in the situation you are testing them? We need to know that first before we inform someone it is wrong or is not happening!
So lets put this a little bit into some context. A classical way to reduce knee valgus or abduction during gait is to fire the glute 'complex' sometimes specifically the glute med. This will create concentric force to abduct the hip to reduce the knee 'falling in'. This occurs in the front foot (pronation) phase of gait.
So if we want to create abduction then should we not first create adduction? During an energy sensitive, in terms of efficiency, activity such as walking creating an eccentric movement first would help generate elastic energy from both the passive and active muscular components.This means less metabolic energy expenditure. This eccentric activation also creates a subconscious mechanical trigger to produce concentric force to move our centre of mass. This means we can walk and talk and freeing our conscious mind to worry about what we are going to have for dinner.
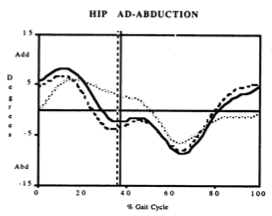
Well this is what happens! But in reverse. When our foot hits the ground we go through an adduction moment at the hip. Don't just believe me, lets refer to a scientific study -
"The hip adducts in the absorption (front foot) phase because the ground reaction force falls medial to the hip and the hip abductor moment is less than the external adduction
moment due to gravitational and acceleration loads" ("Biomechanics of running, T Novacheck 1998). So the external forces outweigh the internal muscular forces.
Novacheck T, Gait and Posture 7 (1998) 77 – 95
Many times an increase in 'gravitational and acceleration loads' can come from a foot that increases pronatory forces. The hip will never have a hope of producing the torque to overcome increased force if it cannot overcome the force in a normal functioning individual with normal pronatory forces occurring.
So we have to ask ourselves if non functional concentric activation or 'firing' into abduction without external forces present (when we are lying on our side or back) is going to help us produce stiffer muscles (resistance to lengthening) that can resist a function related eccentric adduction moment or even an increased adduction moment? Is this even the rationale used? Or are we trying to 'fire' individual muscles such as the glute med (even less chance of overcoming force) to overcome a force we cannot overcome and then blaming a muscle not working?
On an anecdotal note many people who display increased pronation and knee abduction/valgus who I functionally assess seem to lack adduction of the hip. It maybe that the hip muscles/capsule in response to increased force closes down motion. Capsular restrictions many times affect all motions/planes at the hip. Another strategy then maybe to increase the ability of the hip to adduct to help decelerate movement of the femur into adduction. Just because the real bone motion of the femur is towards the mid-line this does not mean the relative hip joint motion is adduction.
Another rationale would be to address the increased force occurring at the foot. A rationale rarely used. That's why we see the single leg squat over the 2nd toe, hopefully to teach the body to resist a force greater than it can by 'firing a muscle' that would be in fact out of the functional sequence. From a functional perspective if we do not decrease force through the decelerative lengthening of adduction that the glute/hip will provide, the force coming up from the floor will just be transferred to another structure, possibly the lumbar spine.
This is my humble opinion on the complex subject of muscle 'firing' and its application. As usual more questions are posed than answers given. For more info check out www.facebook.com/corkinetic
Thanks for reading!!!
Ben Cormack
Latest Articles
 If 9 out of 10 interventions are a load of rubbish, what the hell do I DO?August 4, 2022 - 3:29 pm
If 9 out of 10 interventions are a load of rubbish, what the hell do I DO?August 4, 2022 - 3:29 pm Why the advice to “rest” & “remain active” can both be a bit rubbish!December 21, 2021 - 2:38 pm
Why the advice to “rest” & “remain active” can both be a bit rubbish!December 21, 2021 - 2:38 pm Why I HATE discussions about treatment…….June 22, 2021 - 6:58 am
Why I HATE discussions about treatment…….June 22, 2021 - 6:58 am Evidence based practice – Do you love or loathe it?March 29, 2021 - 3:09 pm
Evidence based practice – Do you love or loathe it?March 29, 2021 - 3:09 pm- The myth of exercise prescriptions – It’s probably more trial and error than we care to admitOctober 15, 2020 - 11:43 am
 Education in rehab – WTF does it mean…..?October 1, 2020 - 12:15 pm
Education in rehab – WTF does it mean…..?October 1, 2020 - 12:15 pm
SIGN UP FOR UPDATES